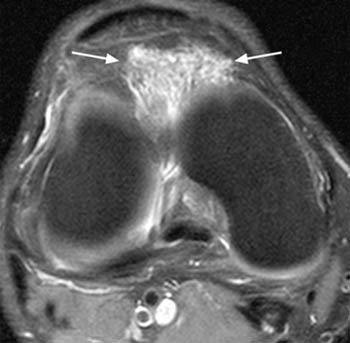
These injuries usually require immediate interventions such as intubation, needle decompression, tube thoracostomy, or pericardiocentesis. Secondary Survey: Potentially Life-threatening Chest Injuries

The injuries to be identified and treated in the thoracic region during the primary survey are:
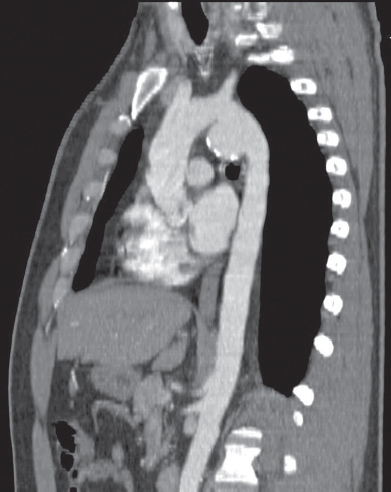
Life-threatening injuries associated with thoracic injuries are often identified in the primary survey by carefully assessing the patient’s ABCDEs. However, in comparison to penetrating trauma, blunt chest trauma patients may have a more subtle presentation with less obvious physical exam findings. There is considerable overlap amongst the various traumatic disorders experienced in both penetrating and blunt chest trauma. By comparison, penetrating trauma largely refers to gunshots, stab wounds, and occasionally impalement. Blunt trauma refers to mechanisms causing increased intrathoracic pressure such as car collisions (most common cause of thoracic trauma), and falls. Thoracic trauma can be distinguished by the mechanism of injury. Unstable chest trauma patients can also deteriorate to the point of traumatic arrest and depending on the mechanism of chest trauma, may be candidates for an emergent ED thoracotomy. Unstable chest trauma patients may show signs of severe respiratory distress or profound shock requiring emergent resuscitation. In patients who are awake and lucid, the chest trauma may present with chest pain, dyspnea, back or abdominal pain, and occasionally syncope. Palpation of crepitus over the chest wall may also be appreciated. In these situations, certain physical examination clues to the presence of trauma include findings such as contusions, lacerations, or deformities. In rare cases, a patient may present in a state of significant altered mental status and be unable to provide any significant history. Unlike other disease entities, trauma patients often present with a known traumatic mechanism such as a car collision, fall, gunshot or stab wound. Trauma patients are commonly encountered in all emergency departments, not just in specified trauma centers. For this reason, emergency medicine providers should be prepared to appropriately evaluate, resuscitate and stabilize any patient with chest trauma. 85-90% of chest trauma patients can be rapidly stabilized and resuscitated by a handful of critical procedures. Chest trauma accounts for approximately 25% of mortality in trauma patients.1,2 This rate is much higher in patients with polytraumatic injuries. As such, any blunt or penetrating trauma can cause significant disruption to each of these systems that can quickly prove to be life threatening unless rapidly identified and treated. The thoracic cavity contains three major anatomical systems: the airway, lungs, and the cardiovascular system.

Discuss the eventual disposition of chest trauma patients based on their diagnosis.List commonly utilized imaging modalities in chest trauma.Generate a differential diagnosis of potential traumatic injuries based on history and physical exam.Describe the components of a primary survey in a chest trauma patient.Identify common pathophysiologic conditions occurring in chest trauma patients.Diagnose, resuscitate, stabilize and manage chest trauma patients.Upon completion of this module, you should be able to: His trachea is noted to be deviated toward the left. There is a large puncture wound to the right, upper anterior chest. On exam, the patient is able to talk but has severely labored breathing. The patient states he feels as though he can’t breathe. The patient states that he was stabbed on the right side of his chest with an unknown object. Kman, MD, OSU Wexner Medical Center Department of Emergency MedicineĪ 21-year-old male presents to the ED by ambulance with complaints of chest pain and shortness of breath that began after he was involved in an altercation outside of a gas station. SAEMF/CDEM Innovations in Undergraduate Emergency Medicine Education GrantĬareer Development and Mentorship CommitteeĬommunications and Social Media CommitteeĪuthor: Nur-Ain Nadir, MD , Nathan Stuempfig, DO Kaiser Permanente Central ValleyĮditor: Nicholas E. Presidential Address: Where Do We Go From Here?ĮMF/SAEMF Medical Student Research Training Grant Virtual Rotation and Educational ResourcesĬommittee Update: NBME EM Advanced Clinical Examination Task Force Visit us on Twitter LinkedIn Facebook YouTubeĮffective Consultation in Emergency Medicine Video
